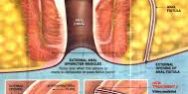
Many factors are capable of causing anal fissures.
The internal anal sphincter is considered to be a smooth muscle that we cannot control. When an anal fissure is present, the internal sphincter is in spasm. Hard feces and bowel movements usually cause a crack in the perianal skin. At the lower end of fissures, a tag of skin may form. Very often, constipation causes a primary trauma. However, several non-traumatic diseases are correlated with anal fissures. The above condition exists especially when a fissure occurs in an unusual location. Many people can remember the exact bowel movement during which their pain began. The pain causes spasm of the anal sphincter which prevents the healing of the tear. Rarely, the fissure can occur after inadequate healing of an anal operative wound.
In addition, inflammatory diseases of the bowel (Crohn’s disease) can be responsible. Among patients with Crohn’s disease, 4% will have an anal fissure as the first manifestation of their Crohn’s disease. Half of all patients with Crohn’s disease eventually will develop an anal ulceration that may look like a fissure. Furthermore, an anal cancer may manifest as a fissure.
In some occasions, a variety of diagnostic tools result in trauma which can produce a fissure. Rectal thermometers, enema tips, endoscopes, or ultrasound probes are some of them.
Other diseases which are capable of causing anal fissures include:
- viral infections (CMV or herpes)
- tuberculosis
- syphilis
- gonorrhea
- chlamydia
- chancroid (Hemophilus ducreyi)
- and human immunodeficiency virus (HIV).
Finally, poor supply of blood to the anus and the anal canal may contribute in the poor healing of anal fissures. Moreover, the increased pressure in the anal canal due to spasm of the anal sphincter may compress the blood vessels there. This results in further reduction of the blood’s flow.